Male Urinary Incontinence & Post Prostatectomy
Bladder Health
What is considered normal?
- The bladder is a storage reservoir that sits right behind the pubic bone.
- Can hold about 2 cups (15-20 oz, or ~750ml) of urine at max capacity
- Normal average voiding time is about 2-4 hours. As we get older, the bladder gets less elastic, capacity decreases, and we need to urinate more frequently. Still usually not more often than every 2 hrs.
- Voiding more often than every 2 hrs may not allow the bladder to fill, and “trains” it to be smaller and get an urge with less volume.
- Urine should flow easily in a good, steady stream until the bladder is empty. No pushing or straining should be needed.
- Most people void about 8-12 oz in a “normal” void, and about 1oz/second, so you should urinate about 8-12 seconds.
- When about 5-6 oz of urine are in the bladder, it stretches and sends an urge signal to the brain. Most of the time, we can ignore that urge for 2+ hrs.
- Urges should not be commands to empty your bladder, just a signal to let you know it’s coming.
- Not all urges happen with a full bladder, and it can be hard to tell the difference!
What are good bladder habits?
- Take your time when emptying your bladder.
- Don’t strain or push, just let it all come out.
- You may need to jiggle or stand up/sit down a time or 2 to make sure it empties all the way.
- Try not to go more often than every 2 hrs, or “just in case”. Again, you don’t always have to go at the first urge. Wait until your bladder is full.
- On the other hand, consistently ignoring the urge and going more than 4 hours isn’t healthy either.
- Urgency and frequency can be improved by retraining the bladder and spacing your fluid intake through the day.
Fluid Intake
- One of the first things people do if they are leaking urine or have strong urge is to not drink as much so they won’t have to pee as much.
- Look at how much you are drinking. For instance, if you’ve just had 2 c coffee, a glass of water with your meds, and then a glass of juice, no wonder you have an urge- that’s a quart of liquid!
- So slow it down. Try drinking the same amount over a longer period of time and see if the same thing happens.
- This can lead to constipation and straining, which can in turn affect urinary leakage.
- Urinary leakage is not an intake problem as much as a storage problem.
- Our bodies need fluid. We are about 90% water. While there is no scientific evidence to support the 8 glasses (64 oz) of water a day, we do need enough to stay hydrated.
- Normally, urine should be pale yellow and have minimal odor. Some medications can change color and odor, so this is not set in stone.
- Most people urinate more in the morning- you haven’t gone as often overnight, moved around less, and then start moving around and have something (often caffeinated) to drink.
- All of this increases the volume of urine in your bladder.
- normal to need to urinate often for the first several hours in the morning.
Constipation
What does constipation have to do with urinary leakage? Actually, a lot.
- Not enough water intake can make stools hard
- Stool in the colon can put pressure on the bladder, increasing urgency
- Straining to have a BM can increase risk of hemorrhoids and weaken the muscles
It is possible to have regular BM or even loose stools and still be constipated. If you have a BM (often fairly well formed), then several hours later have a little more- maybe more pebble shaped, and then some loose, liquidy stool or even smearing, this may be the liquid part oozing around a harder stool up in the rectum/colon.
Despite what your mom told you, you don’t necessarily need to have a BM every day.
- Some people’s digestive systems just move a little slower.
- You should have a “soft, fluffy” stool that is easy to pass without straining.
- You shouldn’t ignore the urge to have a BM. While you don’t always need to go right then, don’t get in the habit of putting it off too long.
- Retrain your system to go at a more convenient time. It is easiest to have a BM about 20-30 min after a meal, as what you just ate stimulates waves of muscle contractions through the intestines to move the food along. The strongest of these waves is in the morning.
- Need about a quart of water a day for good stool consistency
- The longer stool sits in the colon, the more water gets absorbed out, and the harder it gets
When the stool gets down to the rectum, a little bit comes down into the anus and is “sampled” for consistency. The nerves know the difference between liquid, gas, and solid stool. Gas and solid should be able to be held for a little while. The strongest sphincter in the world can’t hold liquid (diarrhea) for more than a few seconds- so find a bathroom fast.
How Diet Can Effect Your Bladder
The following foods may irritate the bladder when consumed in large amounts. Not all of these affect everyone- so it may be some trial and error!
- Alcohol: Reduce to 0-1 drink per day.
- Caffeine (in any caffeinated beverage and some medications): Reduce to 0-1 per day.
- Acid fruit and fruit juices (orange, grapefruit, cranberry, tomato)
- Tomatoes and products containing tomatoes
- Spicy foods
- Milk products
- Raw sugar and added sugar
- Carbonated Beverages: Reduce to 0-1 per day.
- Artificial Sweeteners
Medications that may cause temporary urinary incontinence or make existing incontinence worse, but this doesn’t mean you should go off any of them- just may be harder to gain full control:
Antihistamines Diuretics Anti-psychotics
Sleeping Pills or Sedatives Antispasmodics Decongestants
Anti-Parkinson Agents Antidepressants Calcium Channel Blockers
Be sure to drink enough liquid (water is best). Urine should be clear to pale yellow and have minimal odor if you are well hydrated. Caffeine and alcohol are diuretics- pull fluid from your system and make more urine.
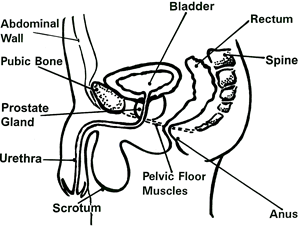
Pelvic Floor Muscles
The pelvic floor muscles form the base of the pelvis and support the pelvic organs (rectum, bladder) and the abdominal contents from above. They act like a trampoline to give support against pressure from above, and “close off the hose” of the urethra and the anus to stop (or start) urine/feces. These muscles work both automatically (we don’t usually have to think about stopping the flow of urine) and voluntarily (we can stop the flow of urine). When they get weak, they generally can’t contract strongly enough to stop the flow of urine- the trampoline “gives” too much. Sometimes when the muscles are weak, they will work extra hard to do their job and get tight or spasmed and painful. In this case, we may need to work on relaxing them first before working on strength.
Men usually don’t have as much trouble with incontinence (leaking urine) because they have a well developed internal sphincter (at the bottom of the bladder), the prostate tends to add some resistance, and the urethra is a lot longer than in women.
Strengthening the muscles takes time- 3-6 months depending on how weak they are! So don’t give up.
The PF muscles should be able to contract, relax, and lengthen/bulge. The surface layer forms a figure 8 around the urethra and anus opening, and when they contract, they close the openings.
- Should feel a slight movement of the penis
- May feel your testicles pull up “nuts to guts”
- Should feel tightening around the anus
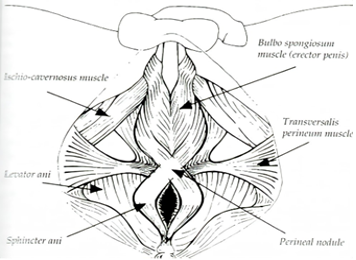
The deeper layer muscles form a hammock or trampoline that resists pressure from above with coughing, sneezing, lifting etc. Contracting these muscles gives more of a drawing in feeling, and the tailbone should move slightly towards the pubic bone. You should also feel the lower abdominal muscles tensing slightly.
With relaxation, the muscle tension should decrease, and the muscles gently lower back to “normal”.
Lengthening/bugling happens when you push to have a BM- the muscles elongate.
Postural Muscles
Many muscles in our body function all day long to keep us upright against gravity. We rarely notice that these muscles are even working as they perform at very low intensity. The lower abdominal and pelvic floor muscles are included in this group of muscles along with muscles such as your back and neck muscles.
The Core and Abdominals
The trunk is a cylinder with the diaphragm at the top, abdominal and back muscles around the middle, and pelvic floor on the bottom. All muscles must work together to distribute pressure and load across the trunk. If one part of the cylinder is weak, pressure pushes out there. This cylinder is commonly also known as the “core”. The deepest of the 4 sets of abdominal muscles is the transverse abdominis, and contraction of this muscle creates a “drawing in” of the lower abdominal wall. Regular exercise of the core muscles including the pelvic floor should build strength, awareness, coordination and retrain the muscles how to function together. This in turn can be the key to controlling your incontinence problem. The core contractions create an internal girdle to support your bladder and pelvic organs as well as your back/trunk. If you hold your breath and push down and out with activity, you are going to push urine down and out. If you activate the PF muscles and core, the muscles can counteract the pressure from above, and urine stays put.
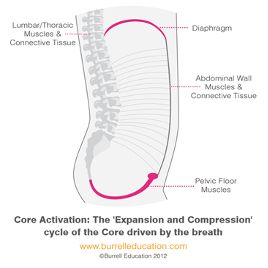
- Strong /well-coordinated abdominal muscles (core) aid the pelvic floor in its function of positioning the urethra and bladder into the pelvic cavity.
- Contracting the abdominal and pelvic floor muscles before and during a cough (or other activity that increases pressure) decreases pelvic floor bulging and urinary leakage.
- Abdominal muscles must work with – not against – the pelvic floor muscles and must be done without holding your breath.
- Breathing patterns can affect the system as well. Normally as the diaphragm lowers during an inhale, the pelvic floor muscles lengthen slightly. Normal exhale is passive, and on forced exhale, both abdominals and PF muscles contract (think blowing out birthday candles).
- The pelvic floor muscles and lower abdominals (transverse abdominis) should normally contract together during all activities, especially lifting.
Pelvic Floor Muscle Contractions (aka Kegels)
Pelvic muscle contractions are used to strengthen the muscles to prevent urine leakage and decrease urgency. They can be done while sitting, standing, or lying down.
How to find the muscles:
- Imagine you are in a crowded room and you feel the need to pass gas.
- Try not to pee; or try to stop the flow of urine
- Imagine pulling the scrotum up inside (“nuts to guts”).
Common errors:
- Breath holding: If you are holding your breath, you may be bearing down against your bladder instead of pulling it up. If your belly bulges up/out while you’re squeezing, you are holding your breath. Try to breathe out gently while performing your PF exercises. This should help encourage those muscles to contract.
- Overdoing it: If you have done too many or held each squeeze too long, your muscles will fatigue and stop working for you. You may actually leak more or feel soreness at the lower abdomen, low back, or rectum.
How many? How often?
Quick flicks. Squeeze the muscle as quick and as hard as you can for one second. Let go for one second.
Long Holds. Squeeze the muscle and hold it. You may need to retighten periodically. Rest between each one, twice as long as you held.
Aggravators. Squeeze your pelvic floor muscle during any activity which would normally make you leak (cough, sneeze, lift, getting out of bed or a chair).
Also do 5-6 quick squeezes with urge to decrease the urge before you walk to the bathroom.
Remember: “Squeeze before you sneeze.” Also known as “the knack”
| Reps. | Hold time | Rest time | |
| Quick flicks | |||
| Long Holds |
Repeat this set of quick flicks and long holds 3-6 times each day.
Work up to 6 sets of 10 quick and 10 long holds per day in standing with emphasis on the front muscles (lift the penis)
Do in any position (sitting, standing, lying)
Challenge your muscles to do more than they are used to doing! Quality is more important than quantity.
Relax and keep breathing during exercises. These muscles are supposed to function automatically.
Overcoming the Urge
Possibly the hardest thing to relearn is to delay the need to urinate. By this point your brain is convinced that if you don’t urinate right now, you will urinate all over yourself, and the muscles may be weak enough that they can’t effectively hold it back, either. The following steps should help, but remember, this didn’t start overnight, and will not go away overnight, so don’t get discouraged and give up, it will get better if you work at it.
When you experience a strong urge to urinate:
- Stop activity, stand quietly or sit down. Try to stay very still to maintain control. Avoid rushing to the toilet.
- Contract your pelvic floor muscles by squeezing and letting go 5 to 6 times to decrease the urge. Pelvic floor contractions send a message to the bladder to relax and hold urine.
- Try to distract yourself by thinking of something other than going to the bathroom. (count backwards from 100 by 7’s)
- Relax. Do not rush to the toilet. Take a deep belly or diaphragmatic breath and let it out slowly. Let the urge to urinate pass by using distraction techniques and positive thoughts.
- Rushing jiggles the bladder, so try to walk normally
- If the urge returns, repeat the above steps to regain control. When you feel the urge subside, walk normally to the bathroom. You can urinate once the urge has subsided.
Urge feeling! -> Stop and be still. -> Do not rush to the toilet. -> Think positively. -> Begin PF contractions. -> Distract yourself.
Post Prostatectomy
Prostate cancer and surgery is a big deal! Despite your small incisions (for robotic/laparoscopic surgery), there was a lot done inside. Removal of the prostate also removes the bottom part of the bladder with the internal sphincter (think of cutting a water balloon above the knot) as well as remove the part of the urethra that goes through the prostate, and then pull the bottom of the bladder down to meet the rest of the urethra.
- It is normal to be 100% incontinent for several weeks after surgery/removal of the catheter
- Some nerve damage is likely, no matter how careful your surgeon is
- This affects nerves to the bladder, pelvic floor muscles, and for erection
- Radiation has its own issues
- The tissues get burned and scarred, and over time can get thinner and more fragile
Be sure to drink enough water. Your incontinence is not a fluid problem, it’s a storage/control problem. We want the bladder to stretch to normal capacity and for the PF muscles to learn to hold again.
Regaining urinary control:
- Most men see improved (not full) control by about 3 months post op, but this can vary!
- It is normal to leak more in the afternoon- you and your muscles are tired
- It is common to leak with lifting, coughing, changing positions or a strong urge
- The pressure from above overcame the ability of the PF muscles to control it
- Some men leak in sitting- this is due to the muscles relaxing a bit, and a little urine just dribbles down the hose from the bladder.
- Before you get up (or cough, laugh, lift…) do a couple PF squeezes
- This keeps urine above the PF muscles from leaking down.
- Anything downstream may still leak out
What should you avoid? Your surgeon will give you specifics, but usually for the first 4-6 wks, avoid lifting more than about 10lbs, straining for BM, high level exercise (lifting weights, running, jumping).
What should you do for exercise? WALK! This will help build endurance and improve blood flow. You may start gentle PF exercises after the catheter is removed.
When can you be sexually active? Not for at least 4-6 wks after surgery. The nerves that control erection have been affected by the surgery. Hopefully you will have some nighttime erections by about 6 wks. You can start self-stroking the penis as early as 2 wks to assist with blood flow- but just gentle, not hard/fast masturbation. You may not have a firm enough erection for penetration for at least 12-18 months. Give yourself time to heal. Many surgeons prescribe Cialis post op- this is more for blood flow for healing than for actual erections, but it helps. The PF exercises will help too. Return of erection varies, and there are options to help when the time comes if you need it.
When can you exercise more vigorously? If you participated in running/jumping sports or heavy lifting prior to surgery, wait until at least 12 weeks (3 months) post op.
- Return gradually- start at about 30% of what you did prior to surgery
- If you ran 3 miles a day before surgery, start walking 1 mile, then gradually run 1 mile
- Stop and back up to lower level if you have discomfort/pain/pressure in lower abdomen or increased urinary leakage
- Your PT can help design an exercise program to safely return to exercise or work activities
Postural Considerations
After abdominal surgery it is common to stay in a bent or flexed posture for comfort. It is important to do some gentle exercise and stand/sit up straight to prevent poor posture from becoming more of a habit.
- Stand against a wall, feet away from the wall, knees slightly bent
- Keep as much of your back and head touching as possible. You may need a towel or pillow behind your head
- Stretch arms out against the wall down by your hips
- Gradually raise arms up until they start to come off the wall like making a snow angel
- Repeat 3-5 times 2-3 times a day
Post Prostatectomy Incontinence
Urinary incontinence post prostatectomy is normal and should gradually improve over time. Most men see improved control by about 3 months but may not be “dry” until as much as 12 months.
Remember that the internal sphincter has been removed along with the prostate, and the urethra shortened slightly (about 1”), so the only way you can control urine is with the PF muscles. Gradually some scar tissue will form at the base of the bladder and that will help slow it down some. The nerves that go to the bladder and pelvic floor muscles have been injured/damaged and take months to heal.
Pelvic floor muscle contractions for exercise as described previously will improve strength and control if you do them consistently. As with any muscle group, it is possible to do too much- and then you may leak more because the muscles are fatigued and sore (think of what your legs feel like if you do too many squats). We want to retrain not only the ability to hold urine so you don’t leak during activity, but also for the bladder to stretch to hold more urine.
Bladder Retraining
The goal of bladder retraining is to get back to more normal pattern of urinating and improve bladder capacity. We can use a schedule of urinating to help improve control and bladder capacity. This will work best if you can be consistent. Don’t give up your pads yet- give yourself a backup.
- Try a voiding diary/log to see what your current pattern is. How often you urinate, leak, and how much you drink.
- Empty your bladder first thing in the morning.
- After that, your schedule will be to wait until the next time you go to urinate.
- Even if you don’t feel you need to go at the next scheduled time, go anyway. Don’t strain but sit/stand and relax. Even if you only get a few drops its ok.
- If you feel the urge before your scheduled time, use the urge delay techniques described earlier.
- If you still have to go, its ok, just try to do the scheduled time the next time.
- The goal is to get to 3-4 hours between urinating
Most information in this HO adapted from Progressive Therapeutics handouts ©2004 used by permission
Pad Weaning Protocol: Jo Milios, PT
As stated earlier, it is normal to be 100% incontinent for the first several weeks after surgery and need to wear heavy absorbency underwear or pads and be soaking them at first. As the nerves and muscles heal, you should be able to gradually wean off the pads.
- Pads starting after surgery during the day
- Use Tena or Depends at night (heavy absorbency underwear)
- 3 dry nights in a row, consider stopping (or going to lighter pad)
- Once dry at night, try delaying pad use in the morning if at home
- Transition to pads only when out, exercising, or at work (6+wks minimum)
- Try no pad morning and evening
- May need a shield (or clamp) for exercise, when out, or with alcohol use
- It is normal to use multiple pads/day for 6+ wks after surgery, and to use liner/shield for even several months after that.
(this table adapted from V. Gaglani)
| Week (post op- minimum) | morning | afternoon | outside |
| 3-4 | Try sitting 10-15 min without pad Heavy ->Medium pads | Heavy pads | Depends->heavy |
| 5-6 | Sit 30-45 min without Med -> light pads | Heavy -> medium | Heavy- > med->none |
| 6+ | Go without 1-2 hrs Light pads | Med-light | Med-light depending on length of outing |
Clamp Protocol: Jo Milios, PT
A penile clamp can be used to assist with training as a way to keep urine from leaking out, especially during activity
- Goals:
- Increase bladder capacity
- Train/strengthen pelvic floor muscles
- Improve quality of life during significant incontinence phase
- Preferably use Weisner (available on Amazon ~$40) or Dribblestop
- Wear during waking hours only
- Start with wearing 2 hrs, then urinate, gradually increasing time between voids (urination) to 3hrs, then to 4 hrs (with clamp in between)
- Don’t go longer than 4 hrs between clamp removal/urination
- Can wear 6 days a week, give 1 day off to rest the skin and test bladder/PF function
- Use either as you are weaning off pads, or instead of pads for exercise/intermittent activity.
- After 4 wks, see how you are doing! May be able to go without if down to 3 pads a day, or go for another 2-4 wks.
- DO NOT USE long term!
Prostatectomy resources
Books:
- “Life after Prostatectomy” Vanita Gaglani, PT
- “Intimacy with Impotence” Ralph Alterowitz
- “Saving your sex life; a guide for men with prostate cancer” John Mulhall
- “Everything You Never Wanted to Know About Erectile Dysfunction and Penile Implants: End Your Silence, Sadness, Suffering, and Shame “ Rick Redner
- “Prostate Recovery MAP: Men’s Action Plan 2” Craig Allingham
Websites:
- “Men have Pelvic Floor Muscles Too…” Pauline Chiarelli, PT (about 1 hr lecture to a community group of prostate CA survivors)
- “Pelvic floor Exercises” Pelvic Floor workshop with Stuart Baptist (westymedia) ~20 min
- “Penile Rehabilitation following Prostate Cancer Surgery” Dr Michael Gillman
- “Physiotherapy Penile Rehabilitation for ED” (use of vacuum pumps)
- “The Diaphragm and the Internal pressure system” Julie Wiebe,PT
www.ustoo.com –prostatectomy support group online
www.pcf.org – prostate cancer foundation
www.pelvicpainrehab.com/blog pelvic floor PT managed website. Good blogs written for patients on variety of pelvic floor topics including prostatectomy, incontinence, and sexual (dys)function
www.lifeafterprostatecancer.com.au
www.drsusieg.com also has a podcast (In Your Pants)
www.thepenisproject.org also has a podcast by the same name
www.mypfm.com geared more towards women, but has a good animated video on “The Basics” of urinary mechanics
www.atouchysubject.com post prostate rehab information and free classes
www.prostate.com.au Prostate CA Center Australia
www.prost.com.au Exercise for prostate cancer
Devices:
- Clamps- Weissner type- Amazon ~$40
- Pumps for ED: ACTIVE erection system
- Andro vacuum pump
Apps For the Phone:
- Squeezy (may also say Squeezy NHS for men)- exercise tracker/reminder. Can set parameters for quick and long hold ex’s,
- Vesica- voiding diary; Healthy Bladder Voiding Diary- diary and will measure urine volume by sound!
- Happify- several modules including chronic pain –relaxation, education…
- Insight timer- guided imagery of 2-40 min duration for relaxation/mindfulness
- Breathe2relax- breathing for relaxation
- Calm- breathing/mindfulness
